Facial Care
Discover Our Aesthetic Treatments for the Face
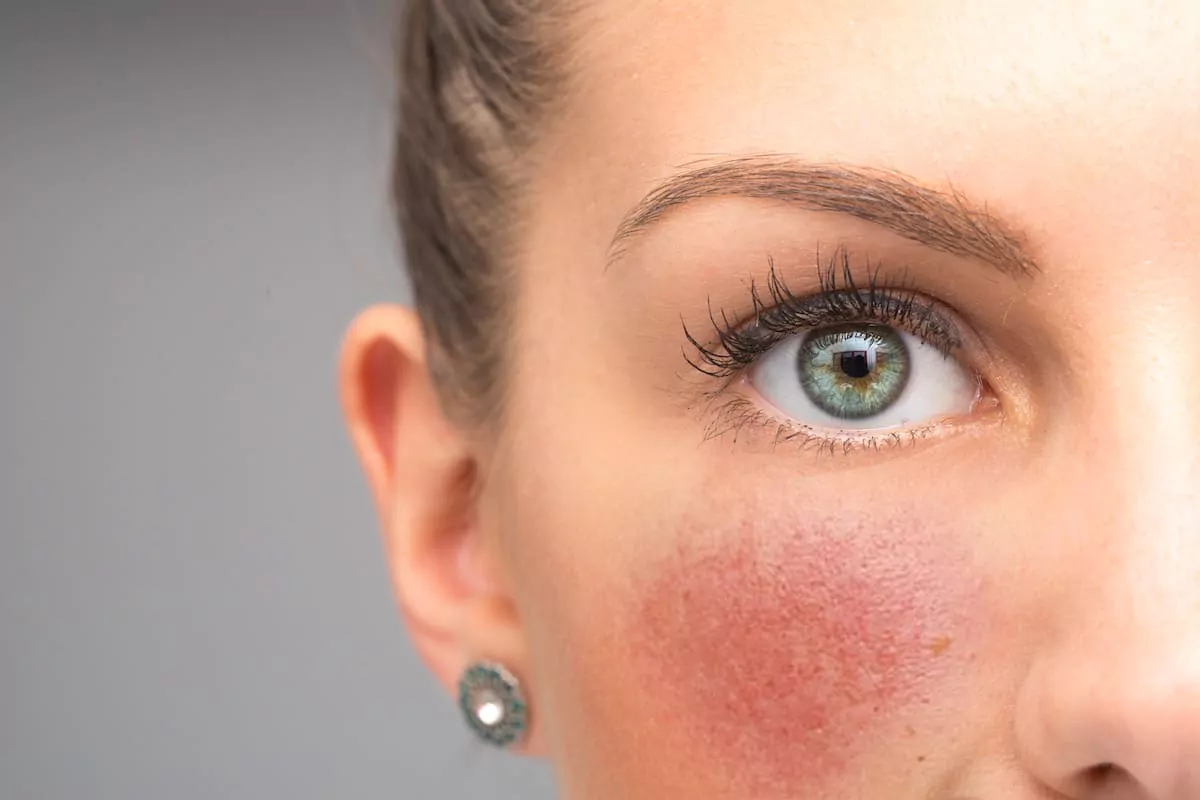
A. FACIAL REDNESS
The term "facial redness" is used when the skin becomes pink, red, bright red, and sometimes even purple or bluish. The redness is due to excessive vasodilation of the blood vessels in a deeper layer of the skin called the dermis, which is the vascularized part located beneath the epidermis. The redness can be localized (nose, cheeks, forehead, or chin) or diffuse, spreading across the entire face.
Depending on their origin, facial redness can be temporary, indicating skin hypersensitivity and lasting only a few moments or a few days. However, when redness persists or occurs more frequently, it is essential to take notice and seek treatment. The psychological and social consequences, aesthetic damage, and negative connotation associated with a "red face" or "flushed appearance" justify seeking medical and aesthetic management of the condition.
B. WHAT ARE THE CAUSES OF THESE REDNESSES?
Facial flushing can be a natural response of the body to strong emotions (anger, excitement, or stress), certain behaviors or situations (physical exercise, allergic reactions, alcohol, hot flashes during menopause, exposure of the skin to excessively high temperatures, etc.). It is a normal response of the body, accentuated and made more visible in individuals with more sensitive, fragile, and/or reactive skin. On normal skin, redness may resolve within a few minutes, but on hypersensitive skin, it may persist for a longer time (a few hours or days). These sudden and transitory redness episodes do not indicate a skin disease and are called flushes or erythema.
Facial redness can also be a sign of various pathologies, the most common being Rosacea. Rosacea is a chronic facial dermatosis that evolves in flare-ups. It affects 2 to 3% of the adult population in France and is more common in women (female/male ratio approximately 2:1). The disease typically starts after the age of 20, with a peak frequency between 40 and 50 years, especially in fair-skinned women. It is almost non-existent in children and beyond a certain age (70 years). In some cases, it can lead to severe forms (conjunctival rosacea, hypertrophic forms, or rhinophyma, especially in men), and pyoderma faciale.
C. DIFFERENCE BETWEEN COUPEROSE, ERYTHROSE, AND ROSACEA?
The terms "couperose" and "rosacea" are often used interchangeably. Rosacea is, in fact, the "official" name of the disease, and couperose is a symptom of rosacea, corresponding to the dilation of blood vessels (visible vessels). Erythrose is characterized by a diffuse and permanent redness.
There are several subtypes of rosacea, including vascular forms (flushes and erythematotelangiectatic), papulopustular forms, and hypertrophic forms. Ocular manifestations affect approximately 30 to 50% of rosacea patients, presenting as dryness, conjunctivitis, blepharitis, photophobia, and even keratitis.
D. VASCULAR FORM OF ROSACEA
This corresponds to paroxysmal vascular phenomena (flushes) or permanent erythematotelangiectatic rosacea.
Temporary Redness (Erythema) or Vasomotor Flushes:
They result from rapid and significant dilation of the cutaneous capillaries. These are paroxysmal facial and neck flushing episodes, accompanied by a local feeling of warmth, without systemic signs, lasting a few minutes. These transient and natural reactions can exacerbate rosacea.
Factors that can trigger flushing include:
Strong emotions, repeated stress, or physical efforts.
Climatic factors: sun exposure, wind (especially cold wind), or cold temperatures.
Sudden changes in temperature, sometimes leading to thermophobia: working near heat sources, hot baths, saunas, and steam rooms (sudden thermal adaptation).
Consuming hot beverages and spicy foods.
Excessive and regular alcohol consumption significantly worsens rosacea and accelerates its progression to erythrosis, couperose, and sometimes severe rosacea or rhinophyma.
A particular clinical form is cortico-induced rosacea, often related to strong and prolonged local corticosteroid therapy on the face. It is characterized by a significant dependence on corticosteroids, dark red to violet desquamative erythema, and multiple telangiectasias. Unlike classic rosacea, the lesions may affect the perioral and/or periocular area.
Erythematotelangiectatic Rosacea:
This is by far the most common form.
The diagnosis is clinical: permanent centrofacial erythema in adults affecting the cheeks, nose, chin, and central part of the forehead, which disappears with digital pressure, associated with telangiectasias predominantly on the sides of the nose and cheeks (couperose).
Swelling (edema) in the center of the face is sometimes visible. The skin may appear dry with desquamation.
Ocular complications are common (30% to 50% of patients have subjective signs): dryness, conjunctivitis, blepharitis, and sometimes keratitis.
a. Erythrosis:
Erythrosis is characterized by a diffuse and permanent redness.
It affects the mid-facial region: cheeks, nose, chin, and the central part of the forehead, sparing the areas around the eyes and mouth. This localization and the permanence of redness are very typical of rosacea. In some cases, it may affect the hairless part of the scalp in balding men.
In this form, redness is accompanied by heightened skin sensitivity, making the application of cosmetics difficult, sometimes even soap and water.
b. Couperose:
The skin coloration may be associated with the development of small, very fine vessels, well individualized on the surface of the skin, very red, and sometimes even purplish, defining the couperose. They are visible just below the skin surface and are referred to as telangiectasias by physicians.
Isolated telangiectasias on the sides of the nose are not a diagnostic criterion.
E. PAPULOPUSTULAR FORM
Long mistaken for acne, the old term "acne rosacea" should be abandoned. Inflammatory papules and pustules appear on a background of permanent erythema with the same topography.
F. HYPERTROPHIC FORM: RHINOPHYMA
It mainly affects men (in over 95% of cases), usually after the age of 50. The nose increases in size, is diffusely red, with dilated follicular orifices. The skin gradually thickens, becoming fibrous, and the nose takes on the classic appearance of "bulbous nose," unrelated to alcohol use. The progression through these successive forms is not obligatory. Surgical treatment or CO2 laser treatment is the only effective approach.
G. WHAT ARE THE CAUSES OF ROSACEA?
- The mechanisms underlying rosacea are still relatively mysterious, and the exact cause of this disease is not known. However, some certainties identified by scientists are:
- Vascular origin of the disease: an anomaly in "shunts" with "hyperactivity" of facial blood vessels. The blood vessels may be functioning abnormally. In rosacea, there can be dysfunction in these veins, leading to blood stagnation in the face's vessels, resulting in vessel dilation, edema, and endothelial alteration, a thin membrane covering the inside of the facial veins. This observation supports the idea of a primary vascularization anomaly.
- Genetic predisposition: The anomaly is mainly found in individuals of Nordic type with fair skin, light eyes, and light hair (which is why rosacea has been called the "Celtic curse"). In France, the disease is rare in the south and much more common north of the Loire River. On the other side of the Mediterranean, especially on dark skin, the disease is practically non-existent.
- The role of Demodex Folliculorum and certain bacteria found in large numbers on the faces of affected patients. Demodex is a saprophytic parasite of the skin flora, including the follicles, also found in perioral dermatitis and post-corticosteroid dermatitis, as well as in blepharitis (inflammation of the eyelids along the eyelash borders). It acts as a pro-inflammatory agent (promotes inflammation) in rosacea.
H. HOW DOES CLINIQUE BIOLASER SAINT-LOUIS/BASEL TREAT COUPEROSE, ERYTHROSE, AND ROSACEA?
- The Laser Saint-Louis/Basel Center offers the most effective solution in treating the vascular forms of rosacea using vascular laser or intense pulsed light (IPL). The laser can reduce the visible redness and telangiectasias of rosacea and reduce the frequency of disease recurrences after laser treatment. The various technological advancements in lasers in recent years have allowed for effective management of couperose and erythrose.
- The light beam emitted by these devices is specifically absorbed by the hemoglobin present in the vessels. This light source generates more or less heat, which causes coagulation (photocoagulation) or destruction (purpura) of the blood vessels.
- The thermo-coagulation mode is a treatment that works well for mild couperose. Usually, 3 to 4 sessions are needed. After the procedure, redness and warmth may last for a few hours.
- The photo-thermolysis mode is preferred for more severe erythro-couperose. It is a more aggressive treatment as it leads to vessel rupture. However, it requires fewer sessions (1 to 2 sessions). This may cause purple purpuric spots (bruise-like appearance) that can last for up to 3 weeks. Social avoidance during this period is recommended. The purpura will completely resolve, changing colors as it heals. In rare cases, hyperpigmentation may persist for a few weeks, especially in individuals with dark, tan, or mixed skin types. For this reason, you will be informed, and potential preparations, sun protection, and photo-protection will be proposed in the weeks following the vascular laser treatment.
- The choice of the most appropriate technique will be determined by the nature of your skin condition, its extent, and your skin type.
I. TREATMENT MODALITIES
Initial Consultation:
- An initial consultation at the center is essential before any treatment.
- You will be provided with an information sheet and a quote.
- Treatment should be performed on clear skin (excluding phototypes V and VI), non-tanned, without any skin lesions in the area to be treated, and no known wound healing disorders.
- Avoid sun exposure for at least 4 weeks before the treatment.
- Day of the Session:
- Each session lasts on average fifteen to thirty minutes. The treatment often requires multiple sessions (2 to 4 on average), spaced 4 to 6 weeks apart.
- The treatment is usually performed without anesthesia on previously cleansed and perfectly clean skin.
- Both the patient and the doctor must wear protective glasses during the treatment.
- A protective gel is applied to the treatment area.
- The laser shot may cause mild discomfort, described as feeling like "elastic band snaps," accompanied by a sensation of warmth but without real pain.
- After the Session:
- In the minutes following the session, your skin will be inflamed (redness, warmth). This may last for a few minutes to a few hours. A hydrating and soothing cream prescribed by the Biolaser center should be applied regularly (at least 3 times a day for 7-10 days).
- Slight swelling may persist for a few days, especially if the treatment was performed under the eyes. You can prevent this by applying cold compresses or an ice pack as soon as you return home and sleeping with your head slightly elevated.
- Small crusts may appear and will disappear in 4 to 7 days while remaining accessible to makeup. They will heal without leaving any traces, thanks to the hydrating cream. Do not scratch or remove them.
- In cases of erythrose (diffuse redness without visible vessels), treatment with purpura may be necessary. In this case, there may be dark red spots or grayish bruises for 15 to 21 days in some areas.
- Pigmentation changes (hypo or hyperpigmentation) usually occur in patients with dark skin or when the treatment area has been exposed to sunlight before or after treatment. Pigment changes usually disappear after 3 to 6 months.
- You can apply makeup to the skin immediately after the session (over the hydrating cream).
- Avoid sun exposure for at least.
- Avoid sun exposure for at least 1 month after treatment. Apply a sunscreen in sunny periods and reapply it every two hours.
J. ROSACEA: REGARDING LOCAL HYGIENE:
- Wash the face with lukewarm water and use cosmetic products suitable for rosacea to conceal redness and improve skin comfort.
- Avoid greasy topicals and occlusive foundations.
- Artificial tears are beneficial in cases of dry eye.
- Photoprotection is useful to prevent recurrences.
- Topical corticosteroids are contraindicated.
- Maintenance treatment with topical metronidazole may be considered in cases of very frequent inflammatory lesion recurrences.
K. RESULTS AND DURABILITY:
- Small blood vessels may disappear immediately after treatment, while larger vessels will gradually diminish in the following weeks.
- On average, a treatment may require 1 to 4 sessions, spaced 1 month apart, depending on the severity of the lesions and the chosen method (photothermolysis with purpura or photocoagulation without notable after-effects).
- Rosacea (erythro-couperose) is a hereditary chronic condition, so maintenance sessions may be necessary in some cases, and the frequency of maintenance will vary from person to person (from several months to several years).










